

Medically Reviewed by Dr P. E. Pancoast, MD
In this article
A simple blood test can provide valuable insight by analyzing critical biomarkers associated with excessive drinking.
If you're curious about how your drinking habits can affect blood test results, it's crucial to understand the impacts alcohol may have on your health.
If you’re getting blood work done, it's best to abstain from alcohol consumption—especially for a fasting blood test. Drinking alcohol can affect blood sugar, cause irregular enzymes and fat levels, and give inaccurate blood test results.
When alcohol is consumed, it can disrupt the balance of glucose regulation in the body, as it impairs the liver's ability to produce glucose and may lead to hypoglycemia.
Additionally, alcohol can alter enzyme activity and fat metabolism in the liver, affecting various blood test components and leading to inaccurate readings, especially in tests that rely on liver function markers and lipid levels.
Avoid drinking alcohol before taking these certain blood tests, especially the night before:
Consult a healthcare professional for more medical advice if you have further questions or want to explore treatment options/resources.
A standard blood test can detect alcohol up to 12 hours after you consume it. But the body may need up to 25 hours to fully metabolize and clear a moderate amount of alcohol from your system.
If you need to fast before a blood test, apart from avoiding food and other beverages, refrain from consuming alcohol for at least 24 hours before it.
But since some blood tests are specific to liver enzymes, it is still best to ask your health provider when you should start avoiding alcohol for your blood test.
Blood tests are one of the most reliable methods for detecting heavy alcohol consumption. They can also effectively measure blood alcohol content (BAC).
Though they can reveal the extent of a person's alcohol intake, blood alcohol tests are only reliable for 6 to 12 hours after the last drink. In general, blood tests help identify the following:
Blood tests are valuable tools used in measuring blood alcohol concentration. Between direct and indirect biomarkers, direct biomarkers are considered more accurate, with an accuracy rate of 99%.
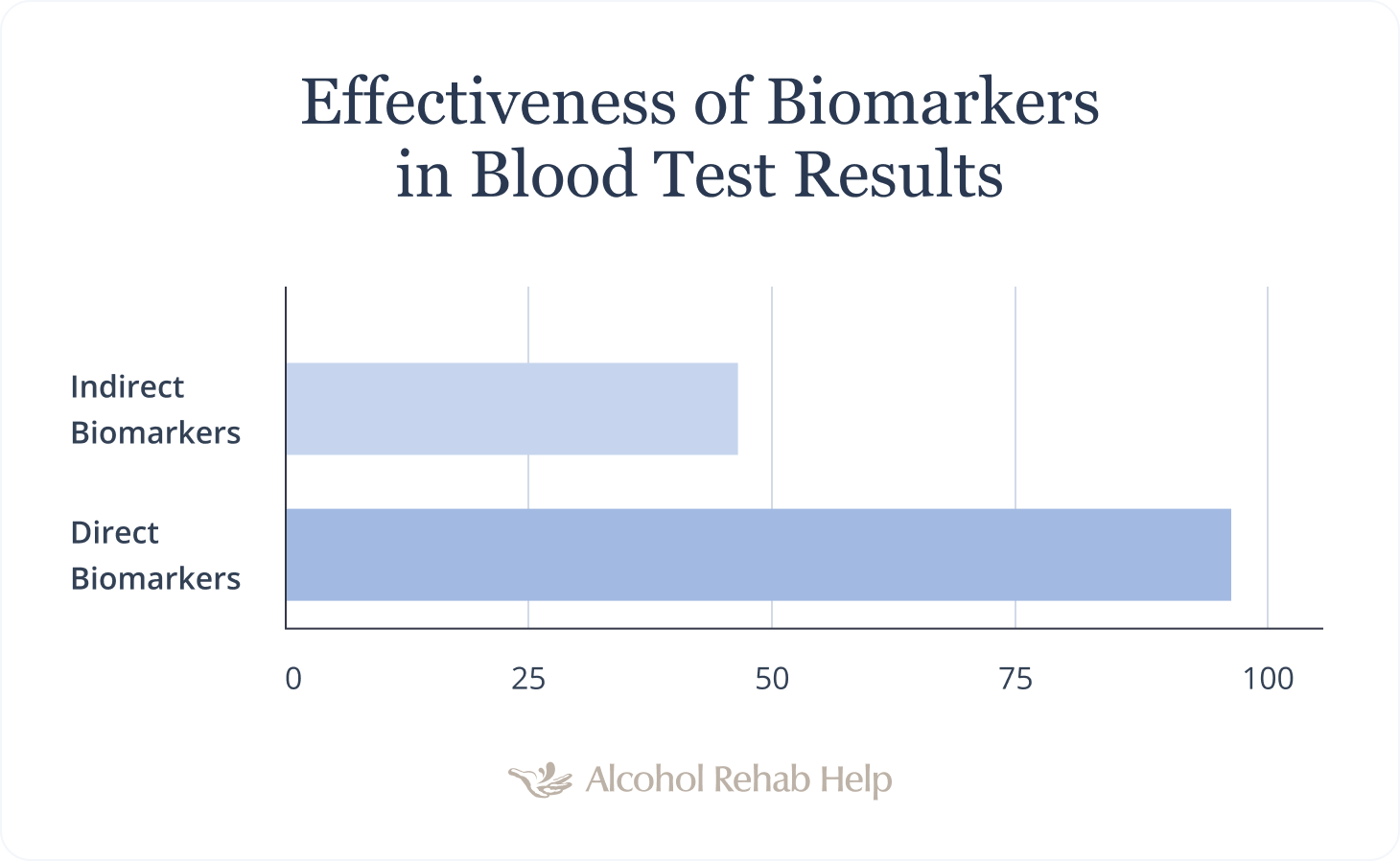
Most blood tests rely on direct and indirect biomarkers, which show how a person’s organs function.
In the past, blood tests relied on indirect markers to determine BAC. In some cases, indirect biomarker tests are as low as 44% accurate.
Direct biomarker testing is approximately 99% accurate. Blood test results for direct biomarkers are even more reliable when confirmed through fingernail and hair testing.
CDT Testing, short for carbohydrate-deficient transferrin, is a blood test used as an alcohol biomarker. These tests help determine if someone is:
Transferrin is a protein in the blood that is crucial in transporting iron throughout the body. When someone drinks too much, it increases certain types of transferrin that are carbohydrate-deficient.
CDT testing measures the amount of carbohydrate-deficient transferrin in a person’s system. Non-drinkers have lower levels of carbohydrate-deficient transferrin.
On the other hand, heavy drinkers tend to have significantly higher levels of it due to their regular consumption of four or more drinks daily (at least five days a week for two weeks before the test).
CDT testing is accurate but not foolproof. This is because heavy drinking doesn’t increase carbohydrate-deficient transferrin for everyone. However, it remains the only test sensitive enough to detect relapse or reduction in alcohol use.
Many therapists use CDT testing to determine a baseline level when treatment begins. If medical professionals suspect someone is drinking with low carbohydrate-deficient transferrin, they encourage follow-up use of other alcohol biomarker tests for the most accurate results.
Other biomarker tests support or disprove the results of a CDT test. The best tests are easy to obtain, inexpensive to evaluate, and acceptable to therapists and those receiving medical treatment.
However, selecting the proper blood test depends significantly on the person undergoing the exam.
The selection of biomarkers may vary based on several factors, including:
Each biomarker testing method has advantages and disadvantages. Many types of biomarkers indirectly indicate blood alcohol exposure or consumption. Age, gender, health status, and ethnicity affect different biomarkers.
Experts recommend using a combination of varying biomarker tests to get accurate results and confirm the status of a person’s alcohol intake.
Million
of Americans suffered Alcohol Use Disorder in 2020.
Percent
of Americans ages 18 and older reported that they engaged in binge drinking.
Million
people have alcohol use disorder (AUD).
In this article

